152 questions match your search.
Which of the following findings is most likely in patients with acute transection of the spinal cord at the level of C6?
- (A) Autonomic hyperreflexia
- (B) Hyperkalemia with administration of succinylcholine
- (C) Hypotension
- (D) Increased pulmonary blood flow
- (E) Tachycardia
Following blunt trauma to the chest, a patient has tachycardia, hypotension, and markedly distended neck veins. Each of the following is expected EXCEPT
- (A) cardiac output of 2.1 L/min
- (B) mixed venous oxygen saturation of 75%
- (C) pulmonary artery occlusion pressure of 25 mmHg
- (D) pulmonary artery diastolic pressure of 25 mmHg
- (E) right atrial pressure of 25 mmHg
A 56-year-old woman with pulmonary fibrosis is scheduled for pneumonectomy. Which of the following parameters best predicts potential postoperative functional impairment?
- (A) Exercise tolerance
- (B) Flow-volume loop
- (C) Resting arterial blood gas values
- (D) Unilateral pulmonary artery occlusion pressure
- (E) Vital capacity and FEV,
A 65-year-old man with essential hypertension well controlled around 140/90 mmHg with hydrochlorothiazide is scheduled for right colectomy for carcinoma. Preoperative EKG and all laboratory values are normal except for a hematocrit of 29% and serum potassium level of 3.2 mEq/L. Central venous pressure (CVP) measured from an internal jugular catheter inserted before induction of anesthesia is 7 mmHg. Ten minutes after induction with thiopental 200 mg followed by enflurane 3% in nitrous oxide and oxygen (50% each), blood pressure decreases suddenly from 110/70 to 80/50 mmHg with heart rate unchanged at 78 bpm. CVP is now 20 mmHg and the EKG demonstrates a midjunctional rhythm. After discontinuing the enflurane, the most appropriate action would be to
- (A) administer furosemide 20 mg intravenously
- (B) verify proper placement of the CVP catheter
- (C) administer atropine 0.4 mg intravenously
- (D) administer packed erythrocytes 1 unit
- (E) administer potassium 20 mEq in 250 ml of intravenous fluid over 15 minutes
Two hours after sustaining extensive burns of the head, neck and chest in a house fire, a patient has stridor and difficulty breathing. The most appropriate management is
- (A) administration of aerosolized epinephrine
- (B) administration of helium and oxygen
- (C) endotracheal intubation
- (D) intravenous injection of dexamethasone
- (E) tracheostomy
A 50-year-old woman develops stridor 10 hours after undergoing thyroidectomy. The most appropriate management is administration of which of the following drugs?
- (A) Albuterol
- (B) Calcium chloride
- (C) Ipratropium bromide
- (D) Racemic epinephrine
- (E) Triiodothyronine
During induction of general anesthesia in a patient with a supraglottic tumor, both intubation and subsequent ventilation via a face mask are impossible. A cricothyroidotomy is performed with a 16-gauge intravenous catheter. Which of the following statements is true?
- (A) Application of pressures greater than 35 cmH2O to the catheter will increase the risk for pulmonary barotrauma
- (B) PaC02 can be maintained at a normal level using a standard circle system attached to the catheter
- (C) PaO2 greater than 100 mmHg can be maintained indefinitely using transtracheal jet ventilation with pure oxygen through the catheter
- (D) Emergency surgical tracheostomy would have improved the likelihood of survival
- (E) The presence of this tumor contraindicates jet ventilation via cricothyroidotomy
A 67-year-old man is undergoing total hip replacement under general anesthesia. He had a permanent endocardial VVI pacemaker placed two years ago for complete heart block, and since arrival in the operating room has been paced continuously. Use of the electrocautery causes the pacemaker to malfunction intermittently. The most appropriate management is to
- (A) tape a magnet over the pacemaker generator and convert to asynchronous mode
- (B) do nothing since the pacemaker is programmed to deal with this circumstance
- (C) stop the surgeon from using the electrocautery
- (D) limit the surgeon to 10 sec/min electrocautery bursts
- (E) place the electrocautery indifferent lead as close as possible to the pacemaker
During laser excision of vocal cord polyps in a 5-year-old boy, dark smoke suddenly appears in the surgical field. The trachea is intubated and anesthesia is being maintained with halothane, nitrous oxide, and oxygen. The most appropriate initial step is to
- (A) change from oxygen and nitrous oxide to air
- (B) fill the oropharynx with water
- (C) instill water into the endotracheal tube
- (D) remove the endotracheal tube
- (E) ventilate with carbon dioxide
A patient with chronic paraplegia (T4 level) is undergoing cystoscopy and removal of bladder calculi without anesthesia. After 10 minutes, blood pressure is 240/100 mmHg and pulse is 50 bpm. The most appropriate management is administration of
- (A) spinal anesthesia
- (B) inhalational anesthesia
- (C) thiopental intravenously
- (D) methyldopa intravenously
- (E) nitroprusside intravenously
During transurethral resection of the prostate, intravascular absorption of glycine irrigant most commonly produces
- (A) alkalosis
- (B) hemolysis
- (C) hypertension
- (D) tachycardia
- (E) wheezing
DC shocks of 200 joules applied directly to the heart are likely to
- (A) worsen coronary perfusion
- (B) prevent postshock arrhythmias
- (C) produce myocardial contractile abnormalities
- (D) increase myocardial impedance
- (E) decrease myocardial temperature
Compared with healthy nonhypertensive patients, in patients with untreated hypertension undergoing anesthesia and operation,
- (A) cerebral ischemia may occur at higher blood pressures
- (B) intravenous fluid should be restricted before induction
- (C) left ventricular hypertrophy enhances compensation for intraoperative fluid loss
- (D) responses to sympathetic stimulation are decreased
- (E) the incidence of intraoperative hypotension is lower
You are called to anesthetize a patient for an emergency pericardial window for a large pericardial effusion. Which of the following drugs is most appropriate for initiation of anesthesia?
- (A) Alfentanil
- (B) Ketamine
- (C) Midazolam
- (D) Propofol
- (E) Thiopental
A 19-year-old college student is brought to the emergency department cyanotic and incoherent. Respiratory rate is 48/min, pulse is 140 bpm, and blood pressure is 140/85 mmHg. The only history obtainable is that he was at a party and suddenly felt sick. Cyanosis persists despite administration of pure oxygen by mask. A venous blood sample is chocolate-brown. The action most beneficial to the patient is to
- (A) intubate the trachea and control ventilation
- (B) perform bronchoscopy to treat foreign body aspiration
- (C) obtain a pulmonary ventilation-perfusion scan
- (D) administer methylene blue intravenously
- (E) administer thiosulfate in normal saline solution intravenously
Which of the following is the most appropriate initial therapy for acute pulmonary hypertension with right ventricular dysfunction and severe systemic hypotension that occurs during anesthesia?
- (A) Amrinone
- (B) Epinephrine
- (C) Isoflurane
- (D) Isoproterenol
- (E) Nitroglycerin
Following pneumonectomy, a paralyzed patient being mechanically ventilated has the following arterial blood gas values: PaO2 71 mmHg, PaCO2 55 mmHg, pH 7.29. SvO2 is 45%. The most likely explanation for this SvO2 is
- (A) decreased red cell mass
- (B) high cardiac output
- (C) hypothermia
- (D) peripheral left-to-right arteriovenous shunt
- (E) ventilation / perfusion mismatch
Which of the following statements concerning myasthenia gravis is true?
- (A) Neostigmine is inappropriate for antagonism of neuromuscular blockade
- (B) The number of acetylcholine receptors is decreased
- (C) Plasma cholinesterase concentration is decreased
- (D) The risk for malignant hyperthermia is increased
- (E) Succinylcholine is contraindicated
Which of the following is the most likely effect of infrarenal cross clamping of the aorta without pharmacologic manipulation?
- (A) Decreased cardiac output
- (B) Decreased pulmonary artery occlusion pressure
- (C) Increased left ventricular stroke volume
- (D) Increased renal blood flow
- (E) Improved myocardial oxygen supply-demand ratio
A 70-kg 61-year-old patient undergoes a four-hour resection of an abdominal aortic aneurysm during anesthesia with fentanyl and enflurane. Infrarenal clamping is required during the procedure. Twelve hours after the procedure, urine output is 15 ml/hr with a fractional sodium excretion of 6%. Which of the following is the most likely cause?
- (A) Enflurane nephrotoxicity
- (B) Hypovolemia
- (C) Intraoperative renal ischemia
- (D) Positive pressure ventilation
- (E) Unilateral ureteral obstruction
A 70-year-old patient is shivering and has chest pain in the PACU following a cholecystectomy. Heart rate is 120 bpm, and blood pressure is 220/120 mmHg. SpO2 is 97% at an FiO2 of 0.4. An ECG shows ST-T wave changes, which are not affected by intravenous administration of nitroglycerin. Which of the following is the most appropriate next step?
- (A) Administration of esmolol
- (B) Administration of hydralazine
- (C) Administration of nitroprusside
- (D) Application of a warming blanket
- (E) Increasing FiO2
Patients with acute alcohol intoxication are at increased risk for each of the following complications of general anesthesia EXCEPT
- (A) aspiration of gastric contents
- (B) hyperglycemia
- (C) hypothermia
- (D) ketoacidosis
- (E) respiratory depression
A patient has a decrease in heart rate from 80 to 50 bpm and a decrease in blood pressure from 140/90 to 60/40 mmHg while in the recovery room after adrenalectomy for pheochromocytoma. The most appropriate treatment is administration of
- (A) atropine
- (B) calcium
- (C) hydrocortisone
- (D) isoproterenol
- (E) norepinephrine
The tracing indicates that the pacemaker generator is
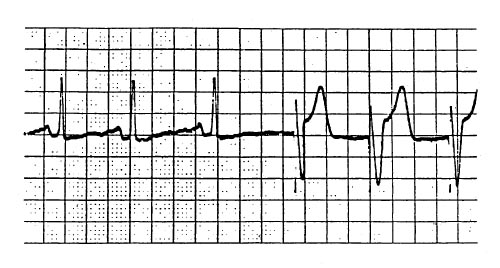
- (A) malfunctioning
- (B) VVT sensing and capturing normally
- (C) VOO sensing and capturing normally
- (D) DVI sensing and capturing normally
- (E) VVI sensing and capturing normally
A 70-kg, 50-year-old man is scheduled for muscle flap closure of a decubitus ulcer over the sacrum. He has been quadriplegic at the level of C6-7 for six years. Which of the following is most likely to result from subarachnoid anesthesia with tetracaine 10 mg for this procedure?
- (A) Atrioventricular block
- (B) Decreased risk for autonomic dysreflexia
- (C) Impaired expiratory muscle function
- (D) Impaired inspiratory muscle function
- (E) Inadequate block of spastic movements
A 55-year-old man who is scheduled to undergo carotid endarterectomy (CEA) has a persistent myocardial filling defect at three hours on a dipyridamole-thallium scan. Which of the following statements is correct?
- (A) Coronary autoregulation is effective in this segment
- (B) Coronary revascularization should precede CEA
- (C) Isoflurane is contraindicated
- (D) Myocardial infarction is impending
- (E) There is a segment of nonviable myocardium
Which of the following statements best describes testing for susceptibility to malignant hyperthermia (MH)?
- (A) Live skeletal muscle cells are required for testing
- (B) The MH gene is located on the X chromosome
- (C) Muscle biopsy is appropriate in children younger than 1 year
- (D) A normal serum creatine phosphokinase concentration eliminates the need for muscle biopsy
- (E) Succinylcholine is used to stimulate muscle obtained on biopsy for MH
A 69-year-old woman with mitral stenosis and atrial fibrillation is scheduled for mitral valve replacement and removal of a left atrial thrombus. After administration of pancuronium, heart rate increases to 140 bpm and blood pressure decreases to 70/40 mmHg. Which of the following is the LEAST appropriate treatment?
- (A) Cardioversion
- (B) Edrophonium
- (C) Esmolol
- (D) Phenylephrine
- (E) Verapamil
A 32-year-old man is scheduled for hernia repair. He underwent heart transplantation for cardiomyopathy five years ago. Which of the following findings is most likely?
- (A) Absence of coronary atherosclerosis
- (B) Biventricular hypokinesis on echocardiography
- (C) Down-regulation of cardiac beta-adrenergic receptors
- (D) Increased heart rate at rest
- (E) Right ventricular hypertrophy
Each of the following is an effect of electroconvulsive therapy EXCEPT
- (A) increased intracranial blood volume
- (B) increased oxygen consumption
- (C) inhibition of parasympathetic activity
- (D) retrograde amnesia
- (E) stimulation of the sympathetic nervous system
Four days after mitral valve replacement, a 49-year-old, 70-kg woman who has had oliguric renal failure since the operation requires insertion of a Schribner shunt for hemodialysis. Her BUN concentration is 104 mg/dl, serum creatinine is 9.3 mg/dl, serum sodium is 130 mEq/L, and serum potassium is 6.7 mEq/L. During the operation under local anesthesia, diazepam 7.5 mg and morphine 10 mg are administered intravenously to control agitation. Five minutes later while she is sleeping quietly, unifocal premature ventricular contractions appear at a rate of 10 per minute on the ECG monitor. The most appropriate therapy is to
- (A) administer calcium gluconate 250 mg intravenously
- (B) augment ventilation with bag and mask
- (C) administer lidocaine 100 mg intravenously
- (D) administer NaHC03 50 mEq intravenously
- (E) observe only
During cardiopulmonary resuscitation (CPR) in an adult, external chest compression is being performed at the rate of 90/min with 2 inches of sternal depression and a compression-relaxation ratio of 20:80. The most appropriate action is to
- (A) decrease the rate of compression
- (B) increase the duration of compression
- (C) increase the duration of relaxation
- (D) increase the depth of sternal depression
- (E) continue the original pattern of CPR
A 36-year-old woman develops acute airway obstruction 24 hours after total thyroidectomy. The most likely cause is
- (A) bilateral recurrent laryngeal nerve injury
- (B) unilateral recurrent laryngeal nerve injury
- (C) hypocalcemia
- (D) subglottic edema
- (E) tracheomalacia
Which of the following is most likely in a 30-year-old patient with untreated hypothyroidism?
- (A) Cardiac arrhythmias with ketamine administration
- (B) Decreased ventilatory response to hypoxia
- (C) Hypoglycemia
- (D) Increased MAC of inhalational anesthetics
- (E) Peripheral vasodilatation
Each of the following is a recognized complication during a transurethral resection for which glycine is used as an irrigant EXCEPT
- (A) disseminated intravascular coagulopathy
- (B) hemolysis
- (C) hyperammonemia
- (D) shoulder pain
- (E) transient blindness
A 45-year-old patient with chronic alcoholism develops jaundice four days after a cholecystectomy under halothane/morphine general anesthesia. Bilirubin and alkaline phosphatase are elevated, but ALT is only slightly above normal. All values were within normal limits preoperatively. The most likely cause of jaundice is
- (A) opioid-induced spasm of the sphincter of Oddi
- (B) hepatic dysfunction secondary to halothane exposure
- (C) worsening of underlying chronic hepatitis
- (D) extrahepatic biliary obstruction
- (E) acute viral hepatitis
Nitroprusside therapy for hypertension should be discontinued in the presence of
- (A) acute myocardial infarction
- (B) increasing metabolic acidosis
- (C) methemoglobinemia
- (D) mitral regurgitation
- (E) renal failure
A 75-year-old man is confused, restless and disoriented two days after an aortic aneurysm repair. Serum sodium concentration is 112 mEq/L, serum osmolality is low, and urine is hypertonic. The most appropriate treatment is
- (A) restriction of fluid intake
- (B) administration of isotonic saline solution
- (C) administration of hypertonic (3%) saline solution
- (D) administration of spironolactone
- (E) infusion of mannitol 25 g
A 75-year-old, 60-kg man with moderately disabling heart failure secondary to ischemic heart disease is undergoing a transurethral prostatic resection under halothane-nitrous oxide anesthesia. Resection time is 30 minutes, and fluid replacement has been lactated Ringer's solution 500 mL. Although heart rate is unchanged, the arterial pressure monitor used because of his cardiac condition has changed from A to B over the last 15 minutes. The most appropriate management is to
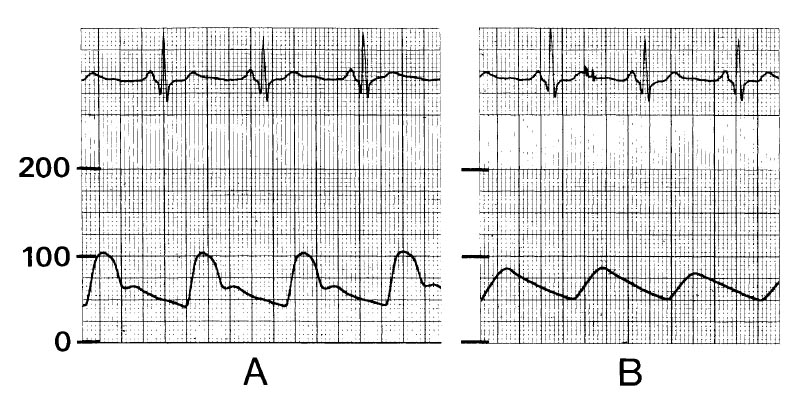
- (A) discontinue halothane
- (B) adminster ephedrine 10 mg intravenously
- (C) administer digoxin one half of his daily dose intravenously
- (D) administer sodium chloride 100 mL of 3%
- (E) do none of the above
Which of the following physiologic changes occurs with immersion in water during extracorporeal shock wave lithotripsy?
- (A) Decreased cardiac output
- (B) Decreased central venous pressure
- (C) Increased expiratory reserve volume
- (D) Increased functional residual capacity
- (E) Increased stroke volume
Which of the following findings on the left is most likely to be associated with an increased risk of complications with cannulation of the left internal jugular vein compared with cannulation of the right internal jugular vein?
- (A) Longer recurrent laryngeal nerve
- (B) Lower location of the cupola of the pleura
- (C) More acute angle between the internal jugular and innominate veins
- (D) More anterior location of the phrenic nerve
- (E) Presence of the thoracic duct
Which of the following statements concerning carbon monoxide poisoning is true?
- (A) Diagnosis is excluded if the PaO2 is greater than 300 mmHg while breathing 100% oxygen
- (B) Increased inspired oxygen concentration accelerates displacement of carbon monoxide from hemoglobin
- (C) Methylene blue decreases binding of carbon monoxide to hemoglobin
- (D) Pulse oximetry accurately reflects hemoglobin oxygen saturation
- (E) Tissue oxygen delivery is normal
Each of the following would be expected in an otherwise healthy 165-kg woman undergoing cholecystectomy EXCEPT
- (A) decreased functional residual capacity
- (B) decreased ventilatory response to carbon dioxide
- (C) increased cardiac output
- (D) increased gastric fluid volume
- (E) increased metabolism of volatile anesthetics
A 57-year-old man has back pain, a heart rate of 90 bpm, decreased pulse in the left arm, and blood pressure of 200/110 mmHg. During infusion of nitroprusside, heart rate increases to 115 bpm and blood pressure decreases to 140/80 mmHg. The most appropriate management at this time is administration of
- (A) droperidol
- (B) nifedipine
- (C) normal saline solution
- (D) propranolol
- (E) verapamil
During a right lower lobe resection, SpO2 decreases from 99% to 70% after institution of one-lung ventilation. FiO2 is 1.0. The most appropriate management is to
- (A) administer an inhaled bronchodilator
- (B) apply continuous positive airway pressure to the right lung
- (C) apply positive end-expiratory pressure to the left lung
- (D) increase tidal volume
- (E) reinflate the right lung
Which of the following postoperative treatments decreases the risk for deep venous thrombosis?
- (A) Blood transfusion
- (B) Epidural anesthesia
- (C) Etomidate
- (D) Ketorolac
- (E) Patient-controlled analgesia
Each of the following improves coagulation in patients with uremia EXCEPT
- (A) conjugated estrogens
- (B) desmopressin
- (C) dialysis
- (D) epsilon-aminocaproic acid
- (E) platelet transfusion
In a patient undergoing liver transplantation, sodium bicarbonate and calcium chloride are administered immediately before reperfusion of the transplanted liver to counteract
- (A) coagulopathy
- (B) decreased cardiac output
- (C) hyperkalemia
- (D) hypermagnesemia
- (E) hypotension
A 25-year-old woman undergoes a difficult open cholecystectomy during anesthesia with isoflurane, nitrous oxide, fentanyl, and vecuronium. Five units of blood are administered intraoperatively. Two days later, the patient has mildly increased serum transaminase concentrations and markedly increased alkaline phosphatase and direct bilirubin concentrations. Which of the following is the most likely cause?
- (A) Acute viral hepatitis
- (B) Hemolysis
- (C) Isoflurane-induced liver dysfunction
- (D) Retained common duct stone
- (E) Sepsis
A 120-kg 56-year-old man undergoing gastrectomy during anesthesia with fentanyl and isoflurane has a PetCO2 of 35 mmHg and a PaCO2 of 50 mmHg. His FEV,/FVC ratio is 80% of predicted. Heart rate is 120 bpm and arterial blood pressure is 80/40 mmHg. Which of the following is the most likely cause of the difference in PaCO2 and PetCO2?
- (A) Aspiration pneumonitis
- (B) Chronic obstructive pulmonary disease
- (C) Decreased cardiac output
- (D) Decreased VD/VT ratio
- (E) Increased QS/QT ratio
Six hours after coronary artery bypass grafting, a pulmonary artery catheter oximeter shows a mixed venous hemoglobin oxygen saturation of 50%. This value may result from each of the following EXCEPT
- (A) anemia
- (B) fever
- (C) hypovolemia
- (D) respiratory alkalosis
- (E) shivering
A 70-kg man with ischemic heart disease is undergoing abdominal aortic aneurysm resection. At the time of infrarenal cross-clamping, 0.2-mV ST-segment depression appears on lead V5 of the ECG. Hemodynamic changes occurring at the same time are shown below. Systemic blood pressure 90/50 --> 150/90; Heart rate 80 --> 95; PAp 20/10 --> 45/24; Mean pulmonary artery occlusion pressure (mmHg) 10 --> 23; Cardiac output (L/min) 4.5 --> 3.2. Ischemia would be decreased by restoring the pre-clamp level of each of the following EXCEPT
- (A) blood pressure
- (B) heart rate
- (C) pulmonary artery pressure
- (D) pulmonary artery occlusion pressure
- (E) cardiac output
The preanesthetic ECG trace (lead II) shown from a 32-year-old woman suggests
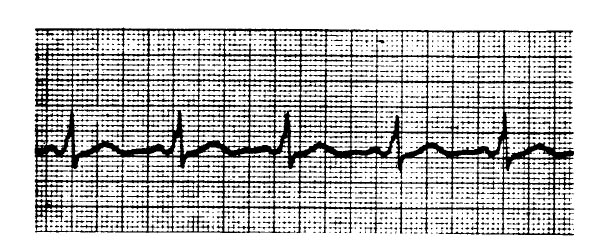
- (A) potential for tachyarrhythmia
- (B) need for preanesthetic atropine
- (C) myocardial ischemia
- (D) left bundle branch block
- (E) right ventricular hypertrophy
A 72-year-old man has massive venous hemorrhage during a radical prostatectomy. Blood pressure decreases from 110/60 to 75/30 mmHg and central venous pressure decreases from 12 to 4 mmHg. PetC02 decreases from 34 to 24 mmHg during constant minute ventilation. The most appropriate next step should be to
- (A) apply positive end-expiratory pressure to the breathing circuit
- (B) attempt to aspirate air from the central venous catheter
- (C) expand intravascular volume
- (D) place the patient in the Trendelenburg position
- (E) turn the patient to the left lateral decubitus position
Which of the following statements concerning autonomic hyperreflexia after spinal cord transection is true?
- (A) It occurs within 24 hours after the injury
- (B) It occurs with lesions below T10
- (C) It is caused by a reflex increase in parasympathetic outflow
- (D) It is characterized by paroxysmal hypotension and tachycardia
- (E) It is prevented by blocking afferent visceral pathways
Each of the following statements concerning the activated clotting time (ACT) is true EXCEPT:
- (A) The ACT is more sensitive than the activated partial thromboplastin time (APTT) to blood heparin concentration
- (B) The ACT is prolonged if the specimen is not warmed during the assay
- (C) The ACT should be greater than 300 sec before initiating cardiopulmonary bypass
- (D) Hypofibrinogenemia may prolong the ACT after cardiopulmonary bypass
- (E) Whole blood is used for measurement of the ACT
Which of the following is a complication of glycine used for irrigation during transurethral resection of the prostate?
- (A) Epileptiform activity on EEG
- (B) Peripheral neuropathy
- (C) Tachycardia
- (D) Transient blindness
- (E) Transient deafness
A patient with alcoholic cirrhosis, ascites, and gastrointestinal bleeding receives 4 units of red blood cells prior to anesthesia with isoflurane in oxygen for emergency exploratory laparotomy. After the peritoneum is opened and the fluid is drained, blood pressure decreases to 60/40 mmHg and SpO2 decreases to 90%. The most likely cause of the hypoxemia is
- (A) acute myocardial ischemia
- (B) decreased 2,3-diphosphoglycerate in transfused blood
- (C) increased intrapulmonary shunting
- (D) relative hypovolemia
- (E) venous air embolism
Two months ago a 68-year-old man with insulin-dependent diabetes mellitus had a transurethral resection of the prostate under spinal anesthesia with tetracaine plus epinephrine. He now has numbness and tingling in both feet and disturbance of gait. Physical examination demonstrates stocking-type hypesthesia of both feet and ankles. The most likely diagnosis is
- (A) anterior spinal artery syndrome
- (B) diabetic neuropathy
- (C) adhesive arachnoiditis
- (D) cauda equina syndrome
- (E) peripheral nerve injury from the lithotomy position
The acute onset of hypotension without a decrease in mixed venous oxygen saturation is most likely associated with the onset of
- (A) hemorrhage
- (B) myocardial infarction
- (C) pulmonary edema
- (D) pulmonary embolus
- (E) sepsis
An endobronchial Robertshaw tube is inserted for resection of a midesophageal tumor under isoflurane, oxygen, pancuronium anesthesia. Forty minutes into a planned two-hour resection, arterial blood gas values are reported as PO2 45 mmHg, PCO2 45 mmHg, and pH 7.33. Ten minutes earlier, the values were PO2 210 mmHg, PCO2, 41 mmHg, and pH 7.39. The first action should be to
- (A) reposition the Robertshaw tube
- (B) apply positive end-expiratory pressure to the ventilated lung
- (C) reinflate and ventilate the non ventilated lung
- (D) increase minute ventilation
- (E) repeat the arterial blood gas analysis
When used for irrigation during transurethral resection of the prostate, glycine 1.5% is associated with each of the following EXCEPT
- (A) hemolysis
- (B) hyperammonemia
- (C) cerebral edema
- (D) hypofibrinogencmia
- (E) visual disturbances
A 72-year-old woman is somnolent one day after left carotid endarterectomy. She has smoked 2 packs of cigarettes daily for 50 years. Six weeks ago, she underwent right carotid endarterectomy. At this time, arterial blood gases while breathing room air are PO2, 45 mmHg, PCO2, 60 mmHg, and pH 7.30. Which of the following is the most likely cause of the increased PCO2?
- (A) Bilateral vocal cord paralysis
- (B) Cerebral infarction
- (C) Congestive heart failure
- (D) Denervation of the carotid bodies
- (E) Phrenic nerve injury
A patient with a fasting blood glucose concentration of 100 mg/dL undergoes a four-hour operation under general anesthesia without intraoperative administration of glucose. On emergence the most likely finding will be
- (A) marked hypoglycemia
- (B) mild hypoglycemia
- (C) normoglycemia
- (D) mild hyperglycemia
- (E) marked hyperglycemia
A 26-year-old patient with multiple trauma is admitted to the intensive care unit postoperatively. The early development of polyuria, hypotension, low urine sodium excretion, high serum osmolality, and normal serum creatinine concentration is best explained by
- (A) adrenal insufficiency
- (B) fluoride-induced high-output renal failure
- (C) inappropriate ADH secretion
- (D) intraoperative fluid overload
- (E) posterior pituitary insufficiency
During transurethral resection of the prostate under spinal anesthesia with a sensory level to T10, a patient has sudden onset of sharp upper abdominal pain and nausea. Arterial blood pressure increases from 120/80 to 150/90 mmHg; the patient becomes diaphoretic. Which of the following is the most likely diagnosis?
- (A) Bladder perforation
- (B) Hemolysis
- (C) Hypervolemia
- (D) Hyponatremia
- (E) Myocardial ischemia
Which of the following situations is most likely related to paraplegia following repair of a descending thoracic aortic aneurysm?
- (A) Decreased cerebrospinal fluid pressure
- (B) Epidural hematoma
- (C) Hypertension proximal to the aortic cross clamp
- (D) Improper placement of surgical retractors
- (E) Prolonged aortic cross-clamp time
Which of the following perioperative interventions decreases the risk for renal insufficiency in patients undergoing aortic aneurysm repair?
- (A) Administration of furosemide
- (B) Administration of mannitol
- (C) Administration of renal-dose dopamine
- (D) Epidural anesthesia
- (E) Preoperative volume expansion
Each of the following statements about pheochromocytoma is true EXCEPT:
- (A) Preoperative administration of alpha-adrenergic inhibitors will usually reverse EKG changes due to catecholamine myocarditis
- (B) Preoperative administration of alpha-adrenergic inhibitors decreases operative mortality
- (C) Beta-adrenergic inhibitors should be administered preoperatively only in conjunction with alpha-adrenergic inhibitors
- (D) Vasopressor therapy may be necessary postoperatively for treatment of hypotension
- (E) Nasal congestion is a sign of inadequate alpha-adrenergic block
A 15-year-old previously healthy boy is scheduled for a celiotomy to relieve an acute intestinal obstruction. A rapid sequence induction is used. Anesthesia is maintained with a balanced technique including nitrous oxide and oxygen (5L:2L), meperidine, and pancuronium. Because of abdominal distention and the high pressure required for inflation of the lungs, a nasogastric tube is inserted. The abdomen remains distended, but compliance improves dramatically. At this time the patient is cyanotic, PaO2 is 48 mmHg, PaCO2 is 52 mmHg, and pH is 7.29. Nitrous oxide is discontinued. The most important therapeutic measure is to
- (A) remove the nasogastric tube
- (B) insert a chest tube on the right side
- (C) withdraw the endotracheal tube 1 cm
- (D) deflate the cuff on the endotracheal tube
- (E) replace the endotracheal tube with one of larger internal diameter
A patient undergoes thoracotomy in the lateral decubitus position. Which of the following maneuvers is most likely to increase PaO2 during one-lung ventilation?
- (A) Applying continuous positive airway pressure to the nondependent lung
- (B) Applying positive end-expiratory pressure to the dependent lung
- (C) Increasing inspiratory flow rate
- (D) Increasing the tidal volume
- (E) Increasing the ventilatory rate
A patient who had liver transplantation two years ago now requires general anesthesia for ENT surgery. Minimal rejection has occurred on a regimen of cyclosporine and prednisone. Which of the following is most likely?
- (A) Hypoalbuminemia
- (B) Hypocalcemia
- (C) Episodic hypoglycemia
- (D) Increased serum creatinine concentration
- (E) Prolonged prothrombin time
You are called to a witnessed cardiac arrest where cardiopulmonary resuscitation is being performed. After successful intubation, arterial blood gas values are PaO2 86 mmHg, PaCO2 63 mmHg, and pH 7.25 at an FiO2 of 1.0. The most appropriate management at this time is to
- (A) repeat arterial blood gas analysis using a new specimen
- (B) administer sodium bicarbonate
- (C) administer fluid challenge with 500 ml of normal saline solution
- (D) hyperventilate the patient
- (E) add positive end-expiratory pressure
Which of the following is the LEAST likely cause of a prolonged prothrombin time?
- (A) Chronic warfarin therapy
- (B) Disseminated intravascular coagulation
- (C) Hemophilia A
- (D) Systemic heparinization
- (E) Vitamin K deficiency
An elderly man has an acute dissection of the descending thoracic aorta. Which of the following antihypertensive therapies is most likely to extend the dissection?
- (A) Esmolol infusion
- (B) Nitroglycerin infusion
- (C) Nitroprusside infusion
- (D) Nitroprusside infusion combined with a beta-adrenergic blocker
- (E) Trimethaphan infusion
A 76-year-old man has a leaking abdominal aortic aneurysm. His blood pressure and pulse have remained stable for 15 minutes at 90/60 mmHg and 130 bpm, respectively. His hemoglobin concentration is 11 g/dl, and the EKG shows a left bundle branch block. Induction of anesthesia should proceed
- (A) after a pulmonary artery catheter has been inserted and the pulmonary artery occlusion pressure is greater than 7 mmHg
- (B) when the pulse has decreased below 130 bpm from the rapid transfusion of blood
- (C) when systolic blood pressure has increased to more than 120 mmHg from the rapid infusion of lactated Ringer's solution
- (D) immediately on arrival in the operating room
- (E) when circulatory signs deteriorate or cease to improve with rapid volume expansion
A 70-year-old man who has just undergone an abdominal aortic aneurysm repair under halothane anesthesia develops hypertension, dyspnea, and cyanosis shortly after awakening in the recovery room. Administration of furosemide 20 mg intravenously improves the cyanosis within 10 minutes. This immediate effect of furosemide is best explained by
- (A) inotropic effect from electrolyte shifts
- (B) decreased preload through diuresis
- (C) increased peripheral venous capacitance
- (D) decreased pulmonary vascular resistance
- (E) increased coronary blood flow
An 80-kg, 70-year-old woman is scheduled for a mastectomy. She has a history of congestive heart failure treated with digoxin 0.25 mg daily. Preoperative examination shows a sinus rhythm at 80 bpm and blood pressure of 110/70 mmHg. Laboratory studies show a serum potassium concentration of 4.2 mEq/L and a serum digoxin concentration of 1.5 mcg/ml. Five minutes after induction of general anesthesia, ventricular bigeminy is noted; blood pressure is 85/65 mmHg, SpO2 is 97%, and PetCO2, is 20 mmHg. Which of the following is the most appropriate management?
- (A) Administration of calcium chloride
- (B) Administration of ephedrine
- (C) Administration of lidocaine
- (D) Administration of potassium chloride
- (E) Decrease in ventilation
A patient with moderate hypothyroidism and unstable angina requires urgent coronary artery bypass grafting. Which of the following is most appropriate before proceeding with the operation?
- (A) Initiation of epinephrine infusion
- (B) Intramuscular administration of a barbiturate
- (C) Intravenous administration of triiodothyronine (T3)
- (D) Intravenous administration of thyroxine (T4)
- (E) Treatment of myocardial ischemia
Bronchospasm occurring during anesthesia in a patient with an ileal carcinoid is best treated by administration of
- (A) aminophylline
- (B) dexamethasone
- (C) halothane
- (D) ketamine
- (E) somatostatin
A 38-year-old woman with hyperthyroidism is undergoing open reduction and internal fixation of a fractured humerus with isoflurane anesthesia. Intraoperatively her heart rate increases to 120 bpm with occasional premature ventricular contractions. The most appropriate therapy at this time is to
- (A) discontinue isoflurane
- (B) administer edrophonium
- (C) administer esmolol
- (D) administer lidocaine
- (E) administer propylthiouracil
A 64-year-old man with diabetes mellitus well controlled with NPH insulin undergoes lower extremity revascularization. Following administration of protamine 10 mg, the patient has facial flushing and blood pressure of 60/30 mmHg. The most appropriate initial step in management is administration of which of the following drugs?
- (A) Diphenhydramine
- (B) Epinephrine
- (C) Hydrocortisone
- (D) Norepinephrine
- (E) Phenylephrine
A 23-year-old man who is receiving his first anesthetic has not resumed spontaneous ventilation two hours after receiving succinylcholine. The train-of-four monitor shows no twitch response. Which of the following is the most likely cholinesterase genotype in this patient?
- (A) Atypical : atypical
- (B) Fluoride-resistant : fluoride-resistant
- (C) Fluoride-resistant : silent
- (D) Normal : normal
- (E) Normal : silent
During enflurane anesthesia for colectomy in a 75-year-old man with sepsis, urine output decreases to 10 ml/hr. Heart rate is 120 bpm, blood pressure is 100/50 mmHg, central venous pressure is 10 mmHg, and pulmonary artery occlusion pressure is 15 mmHg. The most appropriate management at this time is to
- (A) measure cardiac output
- (B) increase fluid administration
- (C) infuse dopamine
- (D) administer propranolol
- (E) switch from enflurane to isoflurane
Hypomagnesemia is associated with
- (A) decreased risk for digitalis toxicity
- (B) dysrhythmias sensitive to bretylium
- (C) hypercalcemia
- (D) prolonged succinylcholine blockade
- (E) surgery requiring cardiopulmonary bypass
A 57-year-old man has back pain, a heart rate of 90 bpm, decreased pulse in the left arm, and blood pressure of 200/110 mmHg. During infusion of nitroprusside, heart rate increases to 115 bpm and blood pressure decreases to 140/80 mmHg. The most appropriate management at this time is administration of
- (A) droperidol
- (B) nifedipine
- (C) normal saline solution
- (D) propranolol
- (E) verapamil
The use of glycine as irrigating solution during transurethral resection of the prostate could be associated with each of the following EXCEPT
- (A) ammonia toxicity
- (B) coma
- (C) hemolysis
- (D) hyponatremia
- (E) transient blindness
In patients with head trauma, which of the following factors results in a return of arterial pH toward normal levels after two days of mechanical hyperventilation?
- (A) Decreased renal absorption of hydrogen ions
- (B) Decreased renal blood flow
- (C) Increased PaCO2 with constant minute ventilation
- (D) Increased renal excretion of bicarbonate ions
- (E) Normalized cerebrospinal fluid pH
A 45-year-old man with chronic liver failure is scheduled for liver transplantation. Which of the following preoperative findings is most likely?
- (A) Hypoxemia
- (B) Increased platelet count
- (C) Increased systemic vascular resistance
- (D) Increased serum factor VIII concentration
- (E) Metabolic alkalosis
Reduction of fire hazards during laser surgery of the airway is best accomplished by use of
- (A) continuous mode laser emissions
- (B) a nitrous oxide/opioid/relaxant anesthetic technique
- (C) a polyvinylchloride endotracheal tube and cuff
- (D) topical lidocaine
- (E) saline-filled sponges over exposed tissues
A 40-year-old woman with Graves' disease is undergoing thyroidectomy with 1% isoflurane, 60% nitrous oxide, and oxygen. During surgical manipulation of the thyroid, temperature increases to 38.5°C, heart rate to 160 bpm, and blood pressure to 150/100 mmHg. The most appropriate initial treatment is to
- (A) administer dantrolene sodium
- (B) administer potassium iodide
- (C) administer propranolol
- (D) administer propylthiouracil
- (E) increase the concentration of isoflurane
A healthy 57-year-old man with a ureteral calculus is scheduled for immersion extracorporeal shock wave lithotripsy. Which of the following statements is true?
- (A) Delivery of the shock wave is timed by the R wave of the ECG
- (B) Continuous epidural anesthesia is contraindicated because of the risk for infection
- (C) If a regional technique is used, a T10 sensory level is required for adequate anesthesia
- (D) If general anesthesia is used, high tidal volumes and low respiratory rate are preferred
- (E) Removal of the patient from the bath is accompanied by an increase in blood pressure
A 50-year-old man who takes aspirin and nifedipine is scheduled for thoracotomy with one-lung ventilation. Which of the following is associated with the greatest risk for intraoperative hypoxemia?
- (A) Preoperative withdrawal of nifedipine therapy
- (B) Intraoperative mild respiratory acidosis
- (C) Intraoperative administration of isoflurane
- (D) Intraoperative administration of nitroglycerin
- (E) Intraoperative thoracic epidural morphine
A 90-kg, 59-year-old man with chronic obstructive pulmonary disease is undergoing laparotomy. Mechanical ventilation is being carried out with a fresh gas flow of 2 L/min at a rate of 16/min and tidal volume of 900 ml; I:E ratio is 1:2.5. PaCO2 remains greater than 50 mmHg. Preoperative PaCO2, was normal. Which of the following is the most appropriate next step?
- (A) Adding 10 cmH20 of positive end-expiratory pressure
- (B) Converting to spontaneous ventilation
- (C) Decreasing inspiratory flow rate
- (D) Increasing exhalation time
- (E) Increasing fresh gas flow
During one-lung ventilation, each of the following affects hypoxic pulmonary vasoconstriction in the nonventilated lung EXCEPT
- (A) application of continuous positive airway pressure to the nonventilated lung
- (B) high alveolar pO2 in the ventilated lung
- (C) infusion of isoproterenol
- (D) low mixed venous pO2
- (E) pulmonary hypertension
Two days after total abdominal hysterectomy, a 54-year-old woman develops lethargy followed by seizures and coma. Laboratory studies show a serum sodium concentration of 108 mEq/L and serum osmolality of 225 mOsm/kg. The most appropriate next step in management is administration of which of the following?
- (A) Desmopressin
- (B) Furosemide only
- (C) Saline solution 0.9% only
- (D) Furosemide and saline solution 0.9%
- (E) Furosemide and saline solution 3%
Compared with a normal child, which of the following is expected during inhalation induction in a child with a 2:1 left-to-right intracardiac shunt?
- (A) Decreased rate of rise of alveolar anesthetic tension
- (B) Decreased anesthetic concentration in pulmonary artery blood
- (C) Decreased cerebral blood flow
- (D) Increased anesthetic concentration in vena cava blood
- (E) No difference in time for anesthetic induction
Which of the following factors is the major cause of hypotension following release of the infrarenal aortic cross-clamp during aortic reconstruction?
- (A) Abnormal myocardial function
- (B) Decreased systemic vascular resistance
- (C) Down-regulation of adrenergic receptors
- (D) Increased PaCO2
- (E) Suppression of the renin-angiotensin system
During right upper lobectomy and one-lung ventilation with a double-lumen endotracheal tube, the PaO2 decreases to 40 mmHg. The PaCO2 is 39 mmHg. Which of the following is most appropriate?
- (A) Confirm position of the tube with bronchoscopy
- (B) Apply 5 cmH20 continuous positive airway pressure to the nondependent lung
- (C) Apply 5 cmH20 positive end-expiratory pressure to the dependent lung
- (D) Resume two-lung ventilation
- (E) Clamp the pulmonary artery of the nondependent lung
A 70-year-old man undergoes cross clamping of the aorta for repair of an abdominal aneurysm. Which of the following methods is most appropriate for decreasing hypotension associated with removal of the cross clamp?
- (A) Administration of a phenylephrine bolus when the cross clamp is removed
- (B) Correction of any base deficit with sodium bicarbonate during clamping
- (C) Decrease of anesthetic to allow blood pressure to increase to 20% above preclamp levels
- (D) Volume loading to increase pulmonary artery occlusion pressure prior to removal
- (E) Infusion of dopamine 10 minutes prior to removal
Which of the following complications is the primary cause of neurologic deficit following carotid endarterectomy?
- (A) Global hypoperfusion
- (B) Hypertension
- (C) Hypotension
- (D) Improper shunt insertion
- (E) Thromboembolism
Which of the following statements concerning absorption of irrigation fluid during transurethral resection of the prostate is true?
- (A) Hydrostatic pressure has minimal effect on the amount of fluid absorbed
- (B) Typically 10 to 30 ml of fluid per minute are absorbed
- (C) Use of iso-osmotic solutions decreases the risk of hyponatremia
- (D) CNS complications are independent of the type of fluid used
- (E) Spinal anesthesia to T6 will mask the symptoms of overhydration
A 75-year-old man with aortic stenosis and coronary artery disease has a preinduction heart rate of 68 bpm and blood pressure of 125/70 mmHg. After induction of anesthesia with fentanyl, midazolam, and pancuronium, heart rate is 90 bpm and blood pressure is 85/45 mmHg. ECG shows a new ST-segment elevation in lead II. Which of the following is the most appropriate initial management?
- (A) Ephedrine
- (B) Epinephrine
- (C) Esmolol
- (D) Nitroglycerin
- (E) Phenylephrine
At a body temperature of 30°C, resistance to blood flow increases because of
- (A) increased hematocrit
- (B) increased plasma fibrinogen concentration
- (C) increased viscosity of blood
- (D) rouleaux formation of red blood cells
- (E) sequestration of platelets in portal circulation
Which of the following statements concerning neuroleptic malignant syndrome is true?
- (A) It does not respond to dantrolene therapy
- (B) It is inherited as an autosomal trait
- (C) It is not triggered by succinylcholine
- (D) It occurs after long-term use of L-dopa
- (E) The halothane-caffeine contracture test is negative in susceptible patients
Which of the following statements concerning carbon monoxide poisoning is true? A 38-year-old woman with a large goiter has undergone subtotal thyroidectomy. Airway obstruction is noted immediately after extubation despite normal vocal cord function on laryngoscopy. Which of the following is the most likely explanation?
- (A) Arytenoid dislocation
- (B) Hematoma
- (C) Hypocalcemia
- (D) Recurrent laryngeal nerve injury
- (E) Tracheomalacia
A 64-year-old patient with chronic obstructive pulmonary disease sustained fractures of ribs 4 through 8 on the left one hour ago. Examination shows agitation, heart rate of 120 bpm, respiratory rate of 30/min, and blood pressure of 180/100 mmHg. PaO2 is 70 mmHg and PaCO2 is 35 mmHg on room air. Radiographs of the chest show no abnormalities. Which of the following is the most appropriate immediate management?
- (A) Continuous epidural analgesia using local anesthetics
- (B) Mechanical ventilation
- (C) Infusion of midazolam
- (D) Patient-controlled analgesia with morphine sulfate
- (E) Surgical stabilization of rib fractures
A patient is bleeding excessively after routine transurethral resection of the prostate. Re-exploration discloses diffuse oozing. The most appropriate management is administration of
- (A) platelets
- (B) fresh frozen plasma
- (C) desmopressin
- (D) epsilon-aminocaproic acid
- (E) cryoprecipitate
A patient is undergoing thoracotomy in the lateral position. Five minutes after initiation of one-lung ventilation using a double-lumen tube and 100% oxygen, SpO2 decreases from 100% to 65%. Which of the following is the most appropriate initial step in management?
- (A) Adding continuous positive airway pressure to the nondependent lung
- (B) Adding positive end-expiratory pressure to the dependent lung
- (C) Increasing the tidal volume to the dependent lung
- (D) Resuming two-lung ventilation
- (E) Verifying the position of the double-lumen tube
A 50-year-old patient undergoes subtotal thyroidectomy for Graves' disease. In the immediate postoperative period, he has marked hoarseness but no stridor. The most likely cause of the hoarseness is trauma to the
- (A) external branch of the superior laryngeal nerve
- (B) internal branch of the superior laryngeal nerve
- (C) recurrent laryngeal nerve
- (D) glossopharyngeal nerve
- (E) vocal cords
In the absence of coronary artery disease, isoflurane-induced vasodilation and tachycardia are beneficial hemodynamic goals for which of the following cardiac diseases?
- (A) Aortic regurgitation
- (B) Aortic stenosis
- (C) Asymmetric septal hypertrophy (IHSS)
- (D) Mitral stenosis
- (E) Pulmonary regurgitation
A previously healthy 28-year-old woman scheduled for laparoscopic tubal ligation becomes, agitated and refuses to undergo the procedure after being brought to the operating room. This behavior most likely resulted from preoperative administration of
- (A) droperidol
- (B) cimetidine
- (C) atropine
- (D) meperidine
- (E) midazolam
Which of the following pre-existing conditions predisposes to new-onset third-degree heart block during pulmonary artery catheterization?
- (A) First-degree heart block
- (B) Left bundle branch block
- (C) Sick sinus syndrome
- (D) Sinus bradycardia
- (E) Wenckebach second-degree heart block
A 40-year-old patient has pain following injection of 8 ml of thiopental 2.5% through a right radial artery catheter. His hand remains pink. Which of the following is the most appropriate next step?
- (A) Injection of lidocaine through the catheter
- (B) Injection of nitroglycerin through the catheter
- (C) Injection of papaverine through the catheter
- (D) Right stellate ganglion block
- (E) No intervention
A 35-year-old woman undergoes a one-hour abdominal liposuction procedure under general anesthesia. During the procedure, 2000 ml of crystalloid is administered and 800 ml of fatty tissue is extracted. Thirty minutes postoperatively, blood pressure is 75/40 mmHg and heart rate is 100 bpm; SpO2 is 94% on room air. Which of the following is the most likely cause of these findings?
- (A) Acute systemic vasodilation
- (B) Circulating free fatty acids
- (C) Hypocalcemia
- (D) Inadequate intravascular volume replacement
- (E) Venous fat embolism
Which of the following is the best method of pacing to improve cardiac output in a patient with third-degree heart block?
- (A) VOO
- (B) AOO
- (C) VVI
- (D) DVI
- (E) Transcutaneous
A 30-year-old man is brought to the emergency department after being rescued from a house fire. With the trachea intubated and FiO2 at 1.0, arterial blood gas values are PaO2 495 mmHg, PaCO2 28 mmHg, and pH 7.28. Hemoglobin saturation measured by co-oximeter is 50%. The most appropriate next step is to
- (A) add positive end-expiratory pressure
- (B) add n-acetylcysteine to the inhaled gases
- (C) administer sodium bicarbonate intravenously
- (D) transfuse 2 units of packed red blood cells
- (E) transfer to a hyperbaric chamber
Following extubation after nasotracheal intubation for seven days, a 35-year-old man has fever, facial pain, nasal stuffiness, and purulent nasal secretions. The most likely cause is
- (A) eustachian tube obstruction
- (B) frontal sinusitis
- (C) maxillary sinusitis
- (D) parotiditis
- (E) retropharyngeal abscess
A patient who is paraplegic secondary to spinal cord transection at T3 develops bradycardia and facial flushing during a nephrectomy under general anesthesia with nitrous oxide, fentanyl, and atracurium. The most likely cause of this response is
- (A) release of histamine
- (B) stimulation of the carotid sinus
- (C) release of prostaglandins
- (D) vagal response to peritoneal traction
- (E) release of epinephrine
A patient has hoarseness after undergoing surgery involving the aortic arch. The most likely cause is an injury to which of the following nerves?
- (A) Glossopharyngeal
- (B) Left recurrent laryngeal
- (C) Right recurrent laryngeal
- (D) Left superior laryngeal
- (E) Right superior laryngeal
During insufflation of the peritoneal cavity with carbon dioxide at the start of laparoscopy, heart rate increases to 140 bpm, blood pressure decreases to 70/40 mmHg, and a loud murmur is heard through the esophageal stethoscope. The most appropriate immediate step is to
- (A) administer a vasoconstrictor
- (B) infuse crystalloid solution rapidly
- (C) discontinue the inhaled anesthetic
- (D) insert a central venous catheter
- (E) deflate the abdomen
A 70-year-old man with mild hypertension and aortoiliac occlusive disease is undergoing aortofemoral bypass grafting. Which of the following interventions is most effective in maintaining renal perfusion during infrarenal aortic clamping?
- (A) Infusion of dopamine at 2 mcg/kg/min
- (B) Infusion of sodium nitroprusside
- (C) Intravenous administration of furosemide
- (D) Intravenous administration of mannitol
- (E) Volume loading with crystalloid
Which of the following statements concerning neuroleptic malignant syndrome is true?
- (A) It does not respond to dantrolene therapy
- (B) It is inherited as an autosomal trait
- (C) It is not triggered by succinylcholine
- (D) It occurs after long-term use of L-dopa
- (E) The halothane-caffeine contracture test is negative in susceptible patients
A 19-year-old man is undergoing inguinal herniorrhaphy. He is anesthetized with a spinal block supplemented with midazolam and fentanyl. During the procedure, he has sudden loss of consciousness, profound hypotension, and bradycardia; systolic pressure is 40 mmHg and heart rate is 30 bpm. Cardiopulmonary resuscitation is started. The most appropriate next step is administration of
- (A) atropine
- (B) ephedrine
- (C) epinephrine
- (D) flumazenil
- (E) naloxone
A 20-year-old woman with poorly controlled diabetes mellitus is scheduled for urgent drainage of an abdominal abscess. She received an initial dose of regular insulin 10 units followed by regular insulin 5 units/hr for the past five hours. Laboratory studies show serum sodium concentration 128 mEq/L, potassium 5.4 mEq/L, chloride 80 mEq/L, and glucose 750 mg/dl. The most appropriate perioperative management is
- (A) addition of subcutaneous NPH insulin
- (B) administration of sodium bicarbonate to correct metabolic acidosis
- (C) administration of normal saline solution to correct the presumed hypovolemia
- (D) administration of furosemide to correct hyponatremia
- (E) infusion of 5% dextrose in 0.2% saline solution to prevent hypoglycemia
A 68-year-old man has signs of a coagulopathy after receiving 10 units of packed erythrocytes during emergency repair of a leaking abdominal aortic aneurysm. The most likely cause is
- (A) depletion of factor V
- (B) disseminated intravascular coagulation
- (C) hypothermia
- (D) platelet dysfunction
- (E) thrombocytopenia
The syndrome of inappropriate ADH secretion is characterized by
- (A) ADH secretion unrelated to serum osmolality
- (B) decreased ADH secretion in response to hypovolemia
- (C) highly dilute urine
- (D) hypernatremia
- (E) negative water balance
A 35-year-old woman with systemic lupus erythematosus is admitted to the critical care unit following sudden onset of severe chest pain. Examination shows tachycardia, hypotension, pulmonary edema, and a blowing systolic murmur in the left parasternal region. The most appropriate management is
- (A) aerosol administration of terbutaline
- (B) intravenous infusion of phenylephrine and nitroglycerin
- (C) intravenous infusion of esmolol
- (D) intravenous infusion of epinephrine and nitroprusside
- (E) volume loading with lactated Ringer's solution
A 63-year-old man with a history of congestive heart failure and left ventricular dilation is scheduled for carotid endarterectomy. During carotid cross-clamping, the surgeon requests that systolic blood pressure be increased from 100 to 160 mmHg. Compared with an identical patient with normal left ventricular size, what is the effect of this change in blood pressure on this patient's myocardial oxygen consumption?
- (A) Equal decrease
- (B) Greater decrease
- (C) Lesser increase
- (D) Equal increase
- (E) Greater increase
Each of the following conditions is a complication of mediastinoscopy EXCEPT
- (A) air embolism
- (B) hemorrhage
- (C) injury to the left recurrent laryngeal nerve
- (D) occlusion of the left carotid artery
- (E) tension pneumothorax
Preoperative administration of an alpha-adrenergic blocker for 10 days to patients with pheochromocytoma will decrease
- (A) episodic tachycardia
- (B) hyperglycemia
- (C) hypovolemia
- (D) nasal stuffiness
- (E) postural hypotension
Unilateral or bilateral diaphragmatic paralysis is a complication of each of the following EXCEPT
- (A) surgical ligation of a patent ductus arteriosus
- (B) use of pericardial ice-slush for topical cardiac hypothermia
- (C) stellate ganglion block
- (D) interscalene brachial plexus block
- (E) C6 cervical fracture-dislocation
A 58-year-old man with a history of angina is undergoing resection of an abdominal aortic aneurysm under morphine, nitrous oxide, d-tubocurarine anesthesia. Just before removal of the aortic cross-clamp, heart rate is 74 bpm, blood pressure is 115/70 mmHg, and pulmonary artery occlusion pressure is 7 mmHg. Immediately after removal of the cross-clamp, heart rate increases to 120 bpm, blood pressure decreases to 80/55 mmHg, and pulmonary artery occlusion pressure decreases to 3 mmHg. The V5 lead on the EKG demonstrates sudden ST-segment depression and T-wave inversion. Initial therapy should be
- (A) reapplication of the aortic cross-clamp
- (B) intravenous administration of sodium bicarbonate
- (C) initiation of a phenylephrine infusion
- (D) rapid expansion of blood volume by transfusion
- (E) initiation of a nitroglycerin infusion
Which of the following is the most sensitive indicator of impending renal failure following trauma?
- (A) Central venous pressure
- (B) Creatinine clearance
- (C) Fractional excretion of sodium
- (D) Hourly urine output
- (E) Urine osmolality
Five minutes after initiating one-lung ventilation using a double-lumen endobronchial tube, a 70-year-old patient has a decrease in Sp02 from 99% to 90%. Tidal volume and respiratory rate are unchanged. Fiberoptic bronchoscopy verifies appropriate positioning of the tube. Which of the following is the most likely cause of the desaturation?
- (A) Blood flow to the nondependent lung
- (B) Failure of hypoxic pulmonary vasoconstriction in the dependent lung
- (C) Inadequate filling of the bronchial cuff
- (D) Inadequate minute ventilation
- (E) Surgical manipulation of the nondependent lung
A patient who is scheduled for emergency laparotomy for bowel obstruction has had oliguria for three hours. She has had hypertension for 10 years. Which of the following laboratory findings would indicate preoperative fluid challenge?
- (A) Urine osmolality: 300 mOsm/L
- (B) Urine specific gravity: 1.015
- (C) Urine sodium concentration: 35 mmol/L
- (D) Fractional excretion of sodium: 0.5
- (E) Ratio of urine-to-plasma creatinine concentrations: 8
During laser excision of a vocal cord polyp, the tracheal tube ignites. Which of the following is the most appropriate next step?
- (A) Continue ventilation with air
- (B) Ensure patency of the endotracheal tube
- (C) Extubate the trachea
- (D) Flood the surgical field with saline solution
- (E) Increase the concentration of nitrous oxide
A man with alcoholic cirrhosis and a hemoglobin concentration of 10 g/dl has an intraoperative PaO2 of 75 mmHg at an FiO2 of 0.5. Which of the following is the most likely cause of the low PaO2?
- (A) Anemia
- (B) Decreased cardiac output
- (C) Increased dead space
- (D) Intrahepatic arteriovenous shunts
- (E) Intrapulmonary arteriovenous shunts
When methylmethacrylate is inserted into the femur, each of the following may occur EXCEPT
- (A) monomer metabolic breakdown
- (B) vasodilation
- (C) hypercarbia
- (D) hypoxia
- (E) increased intramedullary pressure
Following a right lower lobectomy, a patient develops a bronchopleural fistula and becomes hypoxic. He is orally intubated and mechanically ventilated with pure oxygen. PaO2 is 65 mmHg, PaCO2 is 70 mmHg, and pH is 7.25. Which of the following will produce the most favorable change in the blood gases?
- (A) Increasing ventilatory frequency
- (B) Increasing suction on the chest tube
- (C) Applying 10 cmH2O positive end-expiratory pressure
- (D) Using a double-lumen tube for differential ventilation
- (E) Starting negative-pressure ventilation
A 39-year-old patient with insulin-dependent diabetes mellitus receives thiopental 250 mg and succinylcholine 80 mg and is ventilated with 0.75% isoflurane in oxygen. Arterial pressure decreases abruptly from 140/100 to 80/50 mmHg while heart rate remains unchanged at 70 bpm. Failure of heart rate to increase most likely results from
- (A) acute hypoglycemia
- (B) autonomic neuropathy
- (C) depression of sinus node function by thiopental
- (D) depression of the baroreflex response by isoflurane
- (E) ganglionic stimulation by succinylcholine
A 70-kg, 77-year-old man Is undergoing left nephrectomy with nitrous oxide, oxygen, fentanyl, and midazolam anesthesia. He has a 90 pack-year history of cigarette smoking and has chronic obstructive pulmonary disease. One hour after incision, expiratory wheezing occurs and peak Inspiratory pressure increases from 35 to 65 cmH20; end-tidal PCO2 is unchanged, but SpO2 decreases from 97% to 88%. The most likely cause is
- (A) endobronchial intubation
- (B) overinflation of the endotracheal tube cuff
- (C) pneumothorax
- (D) pulmonary edema
- (E) pulmonary embolism
Which of the following statements regarding carbon monoxide poisoning is true?
- (A) Breathing 100% oxygen at 1 atmosphere reduces the carboxyhemoglobin half-life
- (B) Effective treatment includes administration of methylene blue
- (C) It is commonly associated with respiratory acidosis
- (D) It is incompatible with a normal Sp02 while breathing room air
- (E) The oxyhemoglobin dissociation curve is shifted to the right
Each of the following conditions is associated with autonomic hyperreflexia in patients with spinal cord injury EXCEPT
- (A) bradycardia
- (B) flushing below the level of injury
- (C) headache
- (D) sweating above the level of injury
- (E) systolic hypertension
After the first 70 minutes of a transurethral resection of the prostate, a 70-year-old man becomes confused and has tachycardia, hypertension, and shortness of breath. Serum sodium concentration is 116 mEq/L. After informing the surgeon that the procedure should be terminated as soon as possible, the most appropriate next step would be to
- (A) administer furosemide
- (B) administer labetalol
- (C) administer 3% sodium chloride
- (D) change the irrigating solution to normal saline
- (E) induce general endotracheal anesthesia
A patient is scheduled for right pneumonectomy. A left-sided double-lumen endobronchial tube is inserted. After the endobronchial side is clamped and both cuffs are inflated, breath sounds are heard only on the left. Which of the following is the most likely cause?
- (A) Herniation of the endobronchial cuff over the carina
- (B) Occlusion of the right upper lobe bronchus
- (C) Placement of the endobronchial lumen in the left mainstem bronchus
- (D) Placement of the endobronchial lumen in the right mainstem bronchus
- (E) Placement of the endobronchial lumen in the trachea
A 33-year-old woman is scheduled for emergency appendectomy under general anesthesia. She has hypertrophic cardiomyopathy and has had two episodes of syncope in the past year. Which of the following statements concerning anesthetic management is true?
- (A) Spinal anesthesia is preferred to general anesthesia
- (B) Deep levels of isoflurane anesthesia are appropriate
- (C) Fluid administration should be restricted
- (D) Phenylephrine is preferred to ephedrine to treat hypotension
- (E) Positive end-expiratory pressure will decrease left ventricular outflow obstruction
A 65-year-old man is disoriented and has a headache and nausea in the recovery room 30 minutes after transurethral resection of the prostate with glycine irrigation performed under spinal anesthesia. Heart rate is 50 bpm and blood pressure is 180/110 mmHg. Which of the following is LEAST likely?
- (A) Decreased serum osmolality
- (B) Serum sodium concentration 132 mEq/L
- (C) Increased serum ammonia concentration
- (D) Bibasilar rales
- (E) Jugular venous distention
During liver transplantation, venovenous bypass from the femoral and portal veins to the axillary vein during cross-clamping of the inferior vena cava
- (A) decreases urine output
- (B) prevents hypothermia
- (C) prevents metabolic acidosis
- (D) requires heparinization
- (E) supports cardiac output
Pulmonary artery occlusion pressure
- (A) does not reliably reflect left ventricular end-diastolic volume when left ventricular compliance is reduced
- (B) inaccurately reflects left atrial pressure when left atrial pressure exceeds 15 mmHg
- (C) is measured at end-inspiration in mechanically ventilated patients
- (D) overestimates left atrial pressure in patients with poor lung compliance
- (E) reflects left atrial pressure only if the catheter tip is located in zone II of the lung
During isoflurane anesthesia, a 45-year-old patient with chronic asthma has wheezing, prolonged expiration, sinus tachycardia of 120 bpm, and premature ventricular contractions. Preoperative medication included cromolyn and theophylline. The most appropriate treatment is to administer
- (A) albuterol aerosol
- (B) aminophylline by intravenous infusion
- (C) cromolyn aerosol
- (D) halothane
- (E) hydrocortisone by intravenous bolus
A 68-year-old man has a permanent DVI pacemaker that has been functioning appropriately. Which of the following is most likely to cause conversion to VOO pacing?
- (A) Electroconvulsive therapy
- (B) Insertion of a pulmonary artery catheter
- (C) Placement of a magnet over the pulse generator
- (D) Use of electrocautery near the pacemaker
- (E) Shivering